Comprehensive Medical Dermatology Care

Meet Our Providers
Call Us
Welcome to Campbell Dermatology and Aesthetics! We are the premier destination for your dermatologic needs in the Willamette Valley and surrounding communities. We are committed to excellence in medical, surgical, and cosmetic dermatology through physician-driven care.
Your Skin Health, Our Priority
Our Values Guide Every Step of Your Care
At Campbell Dermatology & Aesthetics, care goes beyond treatment guided by compassion, integrity, and excellence, we build lasting relationships rooted in trust.
Acne is a near universal skin problem which occurs in all populations. While it is most associated with teenagers, it can be seen in infants, small children, and older adults. The causes of acne are complex in that hormones, metabolism, stress, and genetics play major roles. Cure of acne is often difficult; however, present day treatment regimens are often very effective in controlling and maintaining control. Treatment centers on using topical and oral medications along with any contributing lifestyle changes. Light therapy and chemical peels can also be effective adjunctive treatments for acne.
We provide effective treatment for Rosacea. Symptoms of this condition include a tendency to blush or flush easily, as well as have persistent redness in the center of your face. The symptoms of this condition can be uncomfortable and embarrassing, interfering with your overall quality of life. Physician specialist uses her dermatological expertise to diagnose and treat this condition so you can enjoy clearer, more beautiful skin. She can help you resolve this condition with topical or oral treatments, better skin care, and our advanced laser therapy. To learn more about rosacea or schedule a consultation with Physician specialist, contact our office today.
Rosacea Symptoms
You may not realize that you are suffering with rosacea because it presents many symptoms which can vary greatly from patient to patient. Contact our office for a consultation if you experience:
- Abnormal flushing
- A hot, stinging sensation in your face
- Skin sensitivity and heat, especially accompanied by redness
- Swollen skin
- Pimples and red bumps that look and feel like acne
- Small facial spider veins from damaged blood vessels
- Scaly red patches of skin
- Thick or raised skin, which often occurs around the nose, chin, cheeks, and forehead
- Larger pores
- Impaired vision and dry, stinging eyes
- Flares coinciding with episodes of emotional stress.
You may experience one or many of these symptoms, depending on your unique circumstances and how far your rosacea has progressed.
Diagnosing Rosacea
Because it can produce a wide range of symptoms that often overlap with other skin conditions, we place a priority on proper diagnosis. You may mistake your rosacea for acne, a sunburn, or eczema, but you can’t get proper treatment without an accurate diagnosis. Dr. Campbell understands the complexities of rosacea, and will complete a thorough skin and eye assessment to diagnose your condition. Rosacea is often a chronic life-long condition but it usually responds well to treatment. Also, the sooner it is treated, the better the results will be.
Treatment Options
Once Dr. Campbell has completed the necessary assessment to diagnose your rosacea, she will recommend a course of treatment. Her suggestions will be based on the severity of your symptoms and your particular concerns regarding your skin.
Basic treatment of rosacea always begins with good skin care. As rosacea is an inflammatory condition, proper skin can with quality skin care products are essential. Also, short and long term sun exposure creates a chronic inflammatory reaction which worsens the problem. Therefore, good sun protection is a must.
In addition to this, our treatment options include:
Topical Treatments–To relieve and manage your rosacea symptoms, Dr. Campbell can prescribe prescription topical treatments in the form of medicated creams or serums. The ingredients in these medications have anti-inflammatory properties which reduce irritation and redness.
Oral Treatments–In some cases, Dr. Campbell may recommend oral antibiotics.
Skin Care–Since rosacea can flare up according to your lifestyle habits, changing your skin care regimen may help treat this condition. Our skin care systems can help patients with rosacea.
Laser Treatment–For persistent redness and inflammation, Dr. Campbell can use a precise, powerful beam of light to clear and remove inflammation and enlarged blood vessels. This process typically takes less than half an hour. Most patients require several treatments to diminish their symptoms. Touch-up treatment can help maintain your results.
Dr. Campbell will determine which of these treatments (or combination of treatments) may be right for you after your consultation. Seek Treatment today if you suffer from rosacea, we can help you enjoy smoother, clearer skin.
Contact our office today to learn more about this condition and your treatment options

Psoriasis is one of the most common skin disorders seen at Campbell Dermatology and Aesthetics. Contrary to what is often portrayed in popular media, psoriasis is highly variable and can be challenging to diagnose. It is often a chronic disorder which is often accompanied by a persistent itching and, if on exposed surfaces, socially embarrassing. As psoriasis is highly variable, so are the treatments which include topical creams, good skin care, oral and injectable medications, as well as lasers. Psoriasis, being a genetic disease, often has associated diseases (called comorbidities) such as arthritis, heart disease, and diabetes. We take psoriasis as a whole-body disorder to give you the best treatment plan available for your psoriasis type.
The wart virus is one of the most common of all skin problems with most persons having warts at some point in their lives. Although warts are usually located on the hands and feet of children, they occur at all ages and all skin areas. Often warts resolve on their own or can be treated with OTC salicylic acid. For warts unresponsive to home remedies, they can be treated with prescription wart treatment as well as liquid nitrogen. Often one or more treatments will be used but Wart treatments can take time and patience to cure as there is not one treatment that will remove warts in a given case.
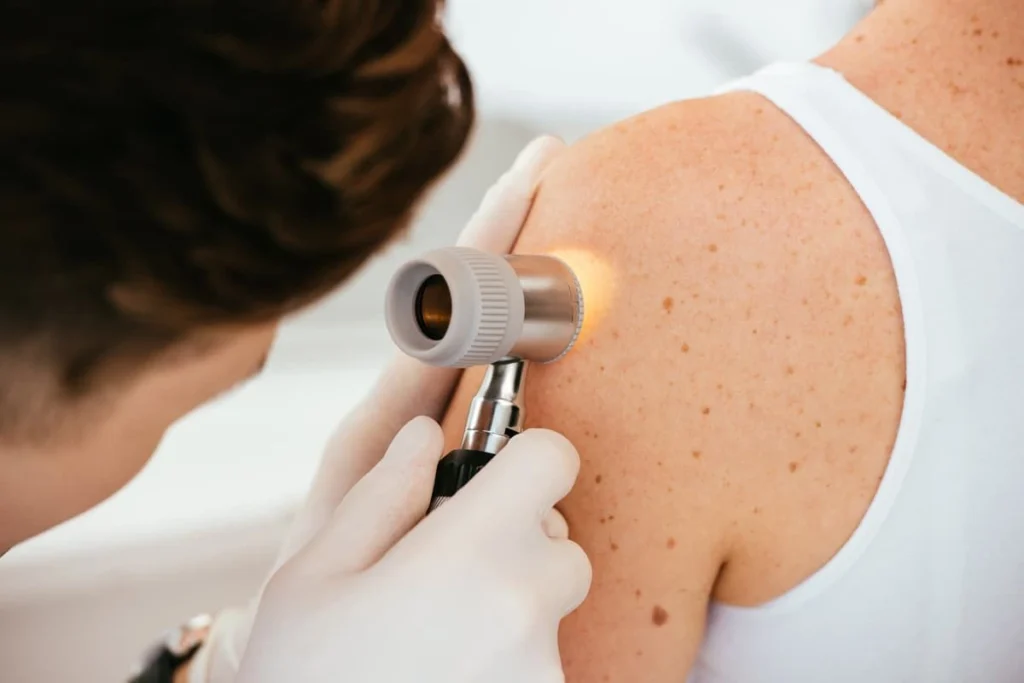
A Pain-Free Cure for Basal and Squamous Cell Skin Cancers
Image Guided-Superficial radiation therapy, or IG-SRT, is a skin cancer treatment offering limited discomfort, no cutting or stitches, and little to no scarring. SRT has emerged as one of the most effective and most sought-after options to treat basal cell carcinoma and squamous cell carcinoma. It also treats non-malignant tumors that cause keloids.
Rather than cutting the cancer from the skin, SRT uses a precise dose of external radiation to destroy the cancer cells. The radiation only goes skin-deep, limiting the risk to healthy internal tissues.
Since the treatment does not involve cutting, bleeding or stitches, there’s little to no pain, low risk of infection, and no need for reconstructive plastic surgery.
There is also no downtime or special precautions following treatment you can continue working and bathing following treatment.
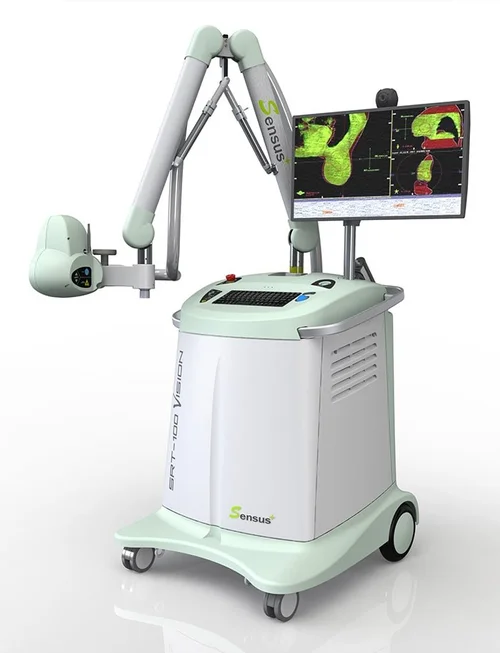
GentleCure is a gentle, surgery-free treatment that is safe and has a 99%+ cure rate in basal and squamous cell skin cancers. Treatment is done right in the dermatology office over the course of a few weeks using an advanced Image-Guided SRT machine. It is the only skin cancer treatment with ultra-sound imaging that lets you see the cancer on the screen and review the progress made throughout the course of the treatment until there are no visible signs of cancer.
More information about SRT here:
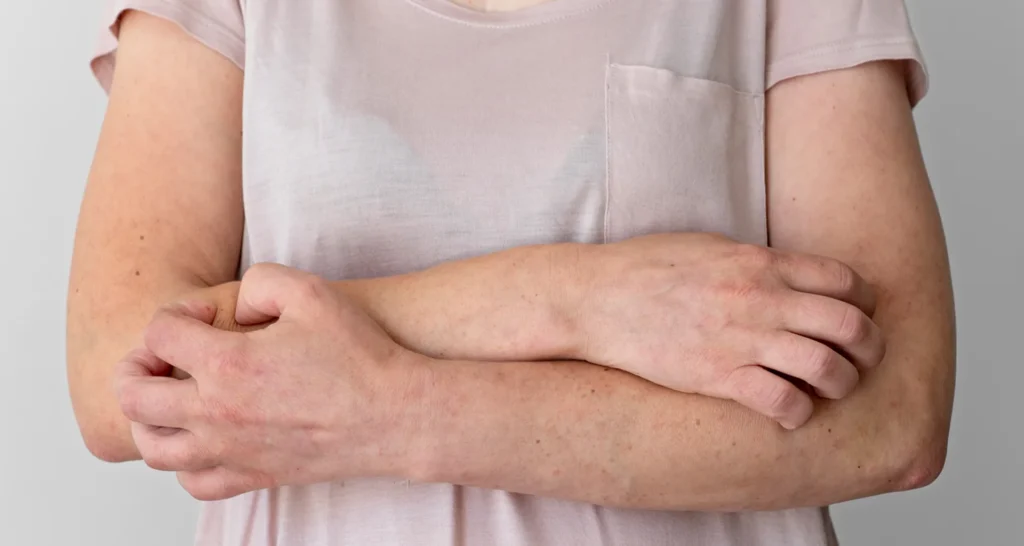
We provide effective eczema treatment, addressing red, itchy, and inflamed skin that impacts daily comfort. Though common at any age, it is especially frequent in children. Physician specialist offers expert diagnosis and personalized care to manage symptoms and restore healthier skin.
Eczema Symptoms
Eczema symptoms can vary widely, ranging from mild irritation to more severe flare-ups. You may experience:
- Persistent itching, often worse at night
- Dry, cracked, or thickened skin
- Red, inflamed, or discolored patches
- Rough or scaly texture
- Small, raised bumps that may ooze or crust over
- Sensitive or swollen skin from scratching
Diagnosing Eczema
Physician specialist evaluates your skin, identifies triggers, and may use allergy testing to create a personalized, long-term eczema care plan.
Treatment Options
While eczema cannot be fully cured, it can be controlled with the right care. Treatment options may include:
- Topical Medications: Corticosteroid or non-steroid creams to reduce inflammation and itching.
- Oral Medications: For more severe cases, prescription drugs to help manage immune response.
- Moisturizers & Skincare: Daily use of emollients and gentle cleansers to strengthen the skin barrier.
- Lifestyle & Trigger Management: Avoiding known irritants, allergens, and stress triggers.
- Advanced Therapies: Light therapy or biologic treatments for resistant eczema.
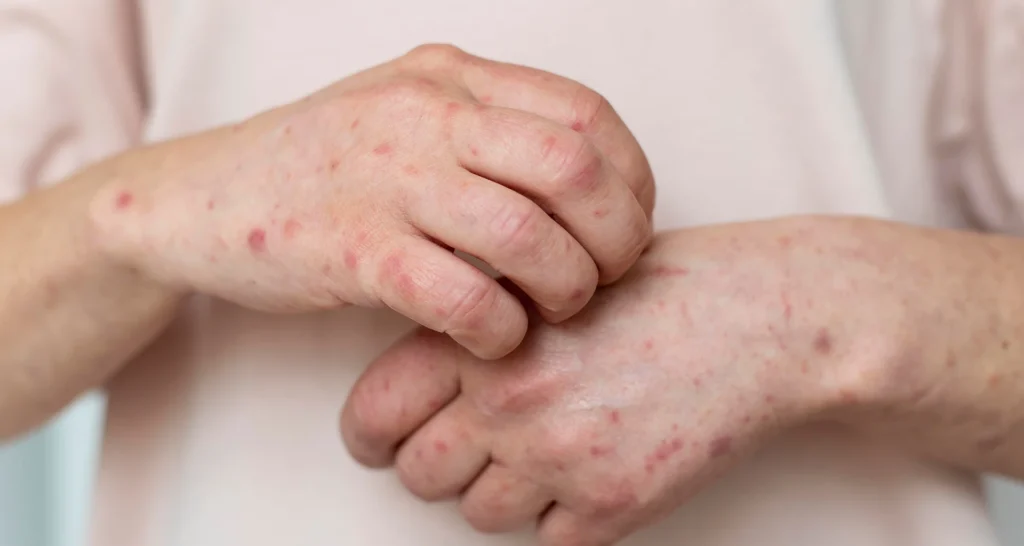
We provide effective treatment for Seborrheic Dermatitis, a common skin condition that causes red, scaly, greasy patches and persistent dandruff. It often affects the scalp, face, ears, chest, and other oily areas of the body. While seborrheic dermatitis isn’t contagious, it can be uncomfortable, long-lasting, and sometimes embarrassing. At Campbell Dermatology, Dr. Campbell combines expert diagnosis with personalized treatment plans to reduce symptoms, control flare-ups, and improve skin health and confidence.
Seborrheic Dermatitis Symptoms
Symptoms may come and go but can include:
- Red, inflamed patches of skin
- Greasy scales or white/yellow flakes (dandruff)
- Itching or burning in affected areas
- Crusty patches on the scalp, eyebrows, or beard
- Flaking and irritation around the nose, ears, or chest
- In infants, thick crusty scales on the scalp (“cradle cap”)
Diagnosing Seborrheic Dermatitis
Dr. Campbell can often diagnose seborrheic dermatitis with a simple physical exam. The appearance and location of the rash are usually enough to confirm the condition. In rare cases, tests may be done to rule out other skin disorders with similar symptoms, such as psoriasis or eczema.
Treatment Options
Seborrheic dermatitis is chronic but manageable. Treatment may include:
- Medicated Shampoos: Antifungal or anti-dandruff shampoos with ingredients like ketoconazole, selenium sulfide, or zinc pyrithione.
- Topical Creams & Ointments: Corticosteroids, antifungals, or calcineurin inhibitors to reduce inflammation and flaking.
- Cleansing & Skin Care: Gentle daily cleansing to reduce oiliness and buildup.
- Lifestyle Management: Avoiding harsh skin products, managing stress, and keeping affected areas clean and moisturized.
- Long-Term Care: Periodic treatment to control flare-ups and maintain healthy skin.
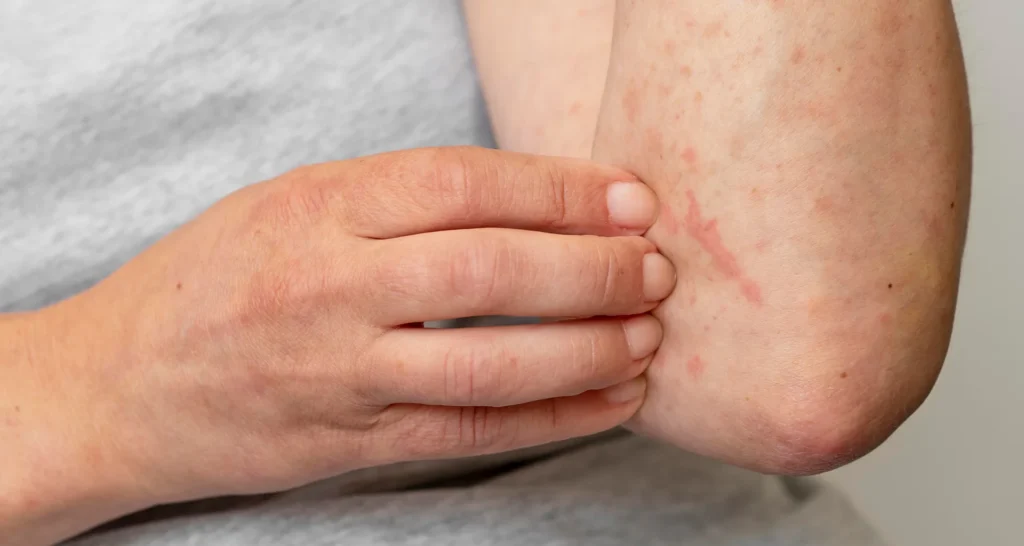
We provide specialized care for Contact Dermatitis, a skin condition caused by direct contact with irritants or allergens. It often appears as an itchy, red rash that can be uncomfortable, painful, and disruptive to daily life. While not contagious, untreated contact dermatitis can lead to ongoing irritation and skin damage. At Campbell Dermatology, Dr. Campbell offers expert diagnosis and personalized treatment plans to identify the cause, relieve symptoms, and prevent flare-ups for healthier skin.
Contact Dermatitis Symptoms
Contact dermatitis may appear within hours or days of exposure and can last for weeks if untreated. Common symptoms include:
- Red rash or bumps on the skin
- Intense itching, which may worsen at night
- Dry, cracked, or scaly patches
- Blisters or oozing lesions in severe cases
- Swelling, burning, or tenderness in affected areas
- Darkened or thickened skin with repeated exposure
Diagnosing Contact Dermatitis
Dr. Campbell diagnoses contact dermatitis through a physical exam and a review of your medical history, including recent exposures to chemicals, products, or environments. In some cases, patch testing may be recommended to identify the specific allergen or irritant causing the reaction.
Treatment Options
Treatment focuses on both relief and prevention:
- Avoidance of Triggers: Identifying and eliminating contact with the irritant or allergen.
- Topical Medications: Corticosteroid creams or ointments to reduce inflammation and itching.
- Oral Medications: Antihistamines or corticosteroids for more severe flare-ups.
- Skin Care Routine: Gentle cleansing, fragrance-free moisturizers, and avoiding harsh products.
- Protective Strategies: Using gloves, barrier creams, and protective clothing to prevent exposure.
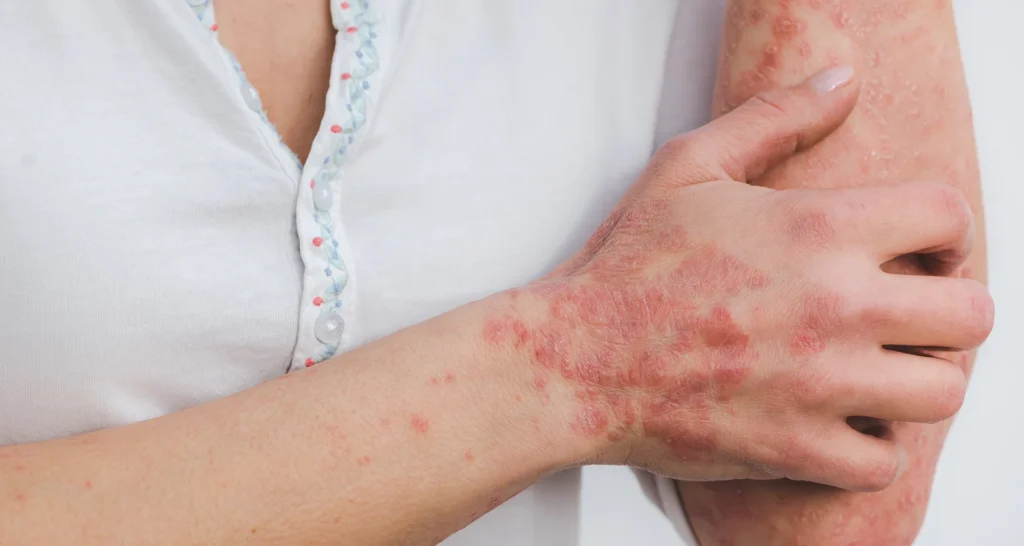
We provide effective care for Hives (Urticaria), a skin reaction that causes itchy, raised welts on the skin. These welts can vary in size, shape, and location, often appearing suddenly and sometimes moving around the body. While hives may resolve on their own, recurring or chronic cases can impact comfort, sleep, and overall quality of life. At Campbell Dermatology, Dr. Campbell offers expert diagnosis and treatment options to relieve itching, reduce flare-ups, and prevent future outbreaks.
Hives Symptoms
Hives can appear anywhere on the body and may last minutes to weeks. Common symptoms include:
- Raised, red, or skin-colored welts (wheals)
- Intense itching or burning sensation
- Welts that vary in size and change shape or location
- Swelling of lips, eyelids, or throat in severe cases (angioedema)
- Symptoms triggered by food, medication, stress, temperature, or environmental factors
Diagnosing Hives
Dr. Campbell diagnoses hives through a physical exam and review of your medical history, including recent exposures and health conditions. For chronic or severe cases, additional testing may be recommended to identify potential allergens, immune responses, or underlying conditions.
Treatment Options
Treatment depends on severity and frequency of outbreaks:
- Antihistamines: First-line treatment to block histamine, reduce itching, and calm welts.
- Oral Medications: Corticosteroids or immune-modulating drugs for severe or persistent hives.
- Trigger Management: Identifying and avoiding foods, medications, or environmental factors that spark outbreaks.
- Lifestyle Guidance: Stress management, gentle skin care, and preventive strategies to reduce recurrence.

We provide comprehensive care for Skin Infections, which can be caused by bacteria, viruses, fungi, or parasites. These infections often lead to redness, swelling, itching, pain, or visible sores and can range from mild to serious. At Campbell Dermatology, Dr. Campbell uses expert evaluation and advanced treatment options to restore skin health, prevent complications, and provide long-term relief.
Skin Infection Symptoms
Skin infection symptoms vary by type but may include:
- Redness, swelling, or tenderness in the affected area
- Warmth and pain around the site of infection
- Pus-filled bumps, blisters, or sores
- Itching, burning, or skin irritation
- Fever, chills, or fatigue in more severe cases
Diagnosing Skin Infections
Dr. Campbell diagnoses skin infections by examining the affected area and, if needed, performing lab tests (such as cultures or swabs) to determine whether the cause is bacterial, fungal, viral, or parasitic. Accurate diagnosis ensures the most effective treatment plan.
Treatment Options
Treatment depends on the type and severity of infection:
- Antibiotic Therapy – Topical or oral antibiotics for bacterial infections like cellulitis, boils, and impetigo.
- Antifungal Treatments – Creams, oral medications, or shampoos to treat fungal conditions like ringworm, athlete’s foot, or yeast infections.
- Antiviral Medications – Targeted therapies for viral infections such as herpes simplex or shingles.
- Lifestyle & Preventive Care – Education on hygiene, wound care, and preventive steps to protect against recurrence.

We provide Full Skin Exams to detect skin cancer and other conditions early, when they are most treatable. During a full-body skin exam, Dr. Campbell carefully evaluates your skin from head to toe, looking for unusual spots, moles, or changes that could signal concern. These routine exams are a key step in protecting your health and maintaining peace of mind.
What is a Full Skin Exam?
A full skin exam is a head-to-toe evaluation of your skin to check for moles, growths, or lesions that could be cancerous or precancerous. Using specialized tools like a dermatoscope, Dr. Campbell examines areas of concern with precision to identify even subtle changes.
Why is it Important?
Skin cancer is the most common form of cancer, and early detection saves lives. Many skin cancers, including melanoma, can be successfully treated if caught early. Full skin exams are especially important if you have risk factors such as:
- A personal or family history of skin cancer
- A large number of moles or atypical moles
- Fair skin, sunburn history, or high UV exposure
- A weakened immune system
What to Expect During Your Exam
- A private, thorough head-to-toe check of your skin
- Careful examination of spots, moles, freckles, or lesions
- Use of dermatoscope magnification for enhanced accuracy
- Education on what to watch for with your own self-checks
- A discussion of any next steps, including biopsy if needed
Treatment & Follow-Up
If an unusual spot or lesion is detected, Dr. Campbell may recommend monitoring, a biopsy, or further treatment. Patients are also guided on sun protection, lifestyle adjustments, and follow-up exams to ensure long-term skin health.

We provide Skin Biopsies to accurately diagnose suspicious spots, rashes, or growths. A skin biopsy involves removing a small sample of skin, which is then examined under a microscope to check for conditions such as skin cancer, infections, or inflammatory skin diseases. This simple, safe procedure gives clear answers and guides the best treatment for your skin health.
What is a Skin Biopsy?
A skin biopsy is a diagnostic test in which a small piece of skin is removed and sent to a lab for analysis. It helps detect skin cancers (like melanoma, basal cell, and squamous cell carcinoma), infections, and chronic skin conditions such as psoriasis or eczema.
Why is it Important?
Skin changes can be caused by many factors, and visual exams aren’t always enough to confirm a diagnosis. A biopsy provides a precise evaluation, allowing early detection and treatment of serious conditions before they progress.
Types of Skin Biopsies
Depending on your condition, Dr. Campbell may recommend one of the following:
- Shave Biopsy – Removes the top layers of skin with a blade.
- Punch Biopsy – Uses a circular tool to remove deeper layers of skin.
- Excisional Biopsy – Removes an entire lesion or growth for evaluation.
What to Expect During the Procedure
- Local anesthesia is used to numb the area.
- The biopsy sample is taken quickly and with minimal discomfort.
- A bandage is applied, and aftercare instructions are provided.
- Results are usually available within a few days.
Follow-Up & Care
Depending on your biopsy results, Dr. Campbell will discuss the next steps, which may include monitoring, medication, or surgical removal if cancerous cells are found. Most biopsy sites heal quickly with minimal scarring.

We provide expert evaluation and treatment for Precancerous Skin Lesions, abnormal skin growths that may develop into skin cancer if left untreated. Early detection and care are critical to preventing progression into more serious conditions. At Campbell Dermatology, Dr. Campbell offers thorough exams, accurate diagnosis, and effective treatment options to protect your skin health.
What are Precancerous Lesions?
Precancerous lesions are abnormal areas of skin where cells show early changes that could eventually become cancerous. Common examples include actinic keratosis, which often appears as rough, scaly patches caused by sun exposure.
Why is it Important?
Not all precancerous lesions progress to cancer, but they carry a higher risk. Detecting and treating these skin changes early prevents them from becoming basal cell carcinoma, squamous cell carcinoma, or melanoma.
Causes & Risk Factors
- Chronic sun exposure or tanning bed use
- Fair skin, light-colored eyes, or a history of sunburns
- Weakened immune system
- Older age
- Family or personal history of skin cancer
Treatment Options
Dr. Campbell tailors treatment based on lesion type and location:
- Cryotherapy – Freezing lesions with liquid nitrogen.
- Topical Medications – Prescription creams to remove abnormal cells.
- Photodynamic Therapy (PDT) – Light-based treatment targeting precancerous cells.
- Surgical Removal – For more advanced or persistent lesions.
Prevention & Skin Health
- Daily use of broad-spectrum sunscreen
- Wearing protective clothing and avoiding peak sun hours
- Regular skin checks at home and professional full skin exams
- Early consultation if you notice new or changing spots

We provide expert care for Sun Damage, which occurs when ultraviolet (UV) rays harm your skin’s DNA, leading to premature aging, wrinkles, sunspots, and increased risk of skin cancer. At Campbell Dermatology, Dr. Campbell helps patients repair visible damage while also protecting against future harm through prevention and personalized treatments.
What is Sun Damage?
Sun damage, also known as photoaging, happens when UV exposure breaks down collagen and elastin in the skin. Over time, this can cause wrinkles, fine lines, leathery texture, sunspots, and a higher chance of developing precancerous lesions or skin cancer.
Signs & Symptoms
- Wrinkles and fine lines
- Sunspots, freckles, or uneven pigmentation
- Rough, dry, or leathery skin texture
- Visible blood vessels (broken capillaries)
- Precancerous lesions (actinic keratosis)
Treatment Options
Dr. Campbell offers both medical and cosmetic treatments to restore skin health:
- Topical Treatments – Prescription creams and retinoids to repair skin damage.
- Chemical Peels & Facials – Remove damaged outer layers and improve skin tone.
- Laser & Light Therapy – Target discoloration, redness, and stimulate collagen renewal.
- Cryotherapy – Freezing precancerous spots such as actinic keratoses.
- Preventive Care – Sunscreen guidance and education to stop further damage.
Prevention & Protection
The best treatment for sun damage is prevention:
- Wear broad-spectrum sunscreen (SPF 30 or higher) daily.
- Avoid tanning beds and excessive sun exposure.
- Wear protective clothing, wide-brimmed hats, and sunglasses.
- Perform regular self-checks and schedule professional full skin exams.

We provide effective treatment for Alopecia Areata. This autoimmune condition causes your immune system to attack hair follicles, leading to patchy hair loss on the scalp, face, and other parts of the body. While it can be distressing and affect self-confidence, treatment can help manage symptoms, encourage regrowth, and improve overall quality of life. Our dermatology team uses advanced diagnostic tools and treatment options to provide personalized care. Learn more below about the symptoms, diagnosis, and treatment options for alopecia.
Alopecia Symptoms
You may notice changes in your hair growth that can vary widely from person to person. Common symptoms include:
- Sudden patchy hair loss on the scalp, beard, or other body areas
- Small, round bald patches that may grow larger over time
- Short hairs that look like exclamation points at the edges of bald spots
- Changes in nails, such as pitting, ridges, or brittleness
- Episodes of regrowth and shedding that can come and go unpredictably
- Total loss of scalp hair (alopecia totalis) or complete body hair loss (alopecia universalis) in severe cases
Diagnosing Alopecia
Diagnosis often begins with a physical examination of the scalp and affected areas. Your dermatologist may:
- Review your medical history and symptoms
- Examine hair and scalp under magnification
- Perform a scalp biopsy if needed
- Run blood tests to rule out other autoimmune conditions
Treatment Options
While there is no cure, several treatments can help stimulate hair growth or reduce the severity of symptoms:
- Topical corticosteroids or injections to reduce inflammation around hair follicles
- Topical immunotherapy to trigger regrowth in resistant cases
- Minoxidil (Rogaine®) to encourage hair regrowth
- Oral medications such as corticosteroids, methotrexate, or newer JAK inhibitors in severe cases
- Lifestyle support and counseling to manage the emotional impact of alopecia

We provide comprehensive treatment for Nail Fungus (Onychomycosis / Fungal Nail Infection). Fungal infections can affect fingernails or toenails, causing them to discolor, thicken, or separate from the nail bed. While often painless, they may become more severe over time — and recurrence is common. Our dermatology team offers evidence-based diagnostic tools and a full range of medical and procedural treatments to help you achieve healthier nails and reduce reinfection risks.
Nail Fungus Symptoms
You might notice one or more of the following:
- Nail discoloration (white, yellow, brown, or sometimes green/black)
- Thickening or misshaping of the nail
- Nail edges that crumble or break off
- Nail lifting or separation from the nail bed (onycholysis)
- A foul odor or debris under the nail
- Gradual progression (the infection often worsens slowly)
Causes & Risk Factors
Common risk factors include:
- Older age (nails become more brittle and slower to grow)
- Wearing tight, non-breathable shoes that trap moisture
- History of athlete’s foot (fungus spreading from skin to nails)
- Walking barefoot in moist public areas (gyms, showers, pools)
- Minor nail or skin injuries that let fungus in
- Underlying conditions: diabetes, poor circulation, weakened immune system
- Nail conditions / skin disorders, e.g. psoriasis, that mimic or predispose to infection
Diagnosing Nail Fungus
Diagnosis typically involves:
- Physical exam and inspection of the affected nail(s)
- Taking nail clippings or scraping debris under the nail for lab analysis (microscopy, culture)
- In some cases, multiple samples or repeat cultures may be needed to confirm the fungus type
- Ruling out other causes (psoriasis, nail trauma, bacterial infections) which can look similar
Prevention & Home Care
Preventing recurrence or spreading of nail fungus is key. Suggestions include:
- Keep nails clean, dry, and trimmed straight across. Smooth edges with a file.
- Disinfect or avoid sharing nail clippers and manicure tools.
- Wear breathable shoes and change socks daily.
- Use antifungal powders or sprays in shoes and between toes.
- Avoid walking barefoot in public, damp places (locker rooms, pool areas).
- If using nail polish, take breaks—you don’t want to trap moisture.
- Promptly treat athlete’s foot or other skin fungal infections.
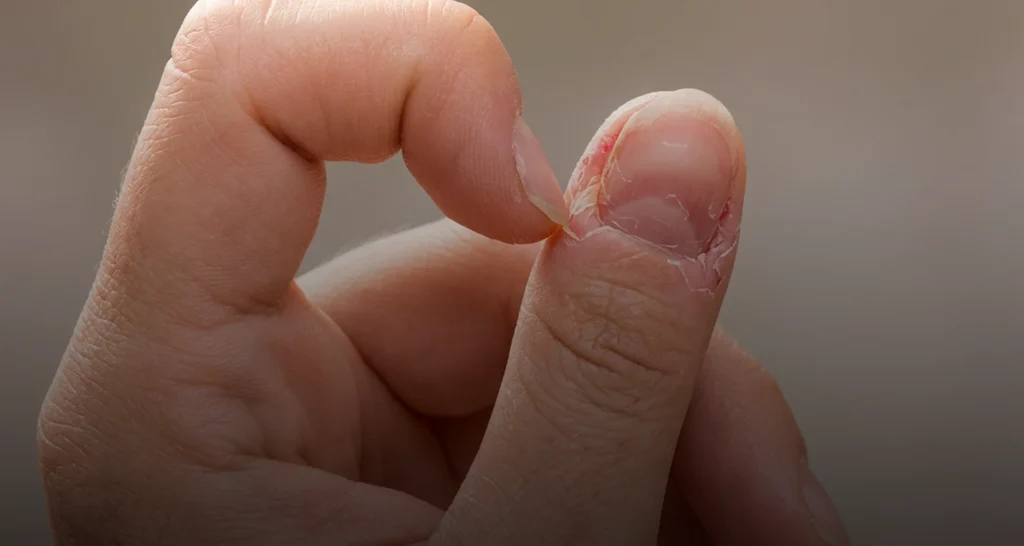
We provide expert diagnosis and care for Ingrown Toenails (Onychocryptosis / Ingrown Nail). When the edge of a toenail grows into the surrounding skin, it can cause pain, swelling, sometimes infection. Though common, it can worsen if left untreated. Our podiatry and dermatology teams use modern techniques to diagnose, treat, and prevent recurrence.
Ingrown Toenail Symptoms
You may experience:
- Pain or tenderness along one or both sides of the toenail
- Redness and swelling around the nail edge
- Infection signs: drainage, pus, warmth
- Hardening of the skin around the nail
- Nail edge digging into surrounding skin or digging deeper over time
- Recurring episodes in the same toe
Causes & Risk Factors
Here are things that can lead to ingrown toenails:
- Cutting nails too short or rounding the corners
- Wearing tight or narrow shoes that apply pressure to the toe
- Repetitive trauma or injury to toes (sports, stubbing, etc.)
- Genetic predisposition (curved nail shape)
- Thickened or deformed nails
- Poor foot hygiene or improperly trimmed nails
- Conditions that increase risk of infection or poor healing (diabetes, circulation issues)
Diagnosing an Ingrown Toenail
Diagnosis typically involves:
- Physical exam: inspecting the toe, skin, nail edges
- Examining signs of infection or tissue changes
- In rare cases, taking a sample of discharge or nail tissue for bacterial/fungal culture if infection is present
- In severe infections, using X-rays to check bone involvement
Treatment Options
Treatment depends on severity and whether infection is involved:
Self-Care & Conservative Methods
- Soak foot in warm water (with Epsom salt or mild soap) twice daily to soften tissue
- Keep toes dry between soaks
- Gently lift the ingrown edge and place a small piece of clean cotton/floss between nail and skin to guide growth above the skin edge
- Use topical antibiotic cream and a light bandage if minor infection signs are present
- Wear roomy shoes or sandals to reduce pressure
Medical / Procedural Options
- Professional trimming and reshaping under sterile conditions
- Partial nail avulsion (removing the ingrown side) under local anesthesia
- Complete nail removal (avulsion) in more severe cases
- Matrixectomy / chemical ablation to prevent regrowth of the problematic edge (e.g. apply phenol or other agents) for chronic recurrence
- Antibiotics if infection is present and not resolved by simple measures
Prevention & Home Care
To reduce the chance of recurrence:
- Trim toenails straight across, not rounded at the edges
- Avoid cutting nails too short
- Use clean, disinfected nail clippers
- Choose shoes that fit well — not too tight, with enough toe room
- Avoid repeated trauma or pressure on toes
- Monitor and treat any fungal or skin conditions that affect the toes
- If you have diabetes or poor circulation, inspect feet daily and seek early care

We provide treatment for Hyperhidrosis, a condition that causes excessive sweating even when it’s not hot or during rest. It can be uncomfortable, affect daily life, and impact confidence. Our team offers advanced options to manage symptoms and improve quality of life.
Hyperhidrosis Symptoms
- Excessive sweating in hands, feet, underarms, face, or back
- Sweating that soaks clothes or drips from skin
- Skin irritation, odor, or peeling in moist areas
- Emotional or social discomfort from sweating
Causes & Risk Factors
- Overactive sweat glands
- Family history of excessive sweating
- Triggers like heat, stress, spicy food, caffeine, alcohol
- Medical conditions or certain medications
Diagnosing Hyperhidrosis
- Review of medical history and symptoms
- Physical exam of affected areas
- Sweat tests to measure severity
- Blood tests if another condition is suspected
Treatment Options
- Prescription-strength antiperspirants
- Medicated wipes or oral medications
- Iontophoresis (water and mild electrical current for hands/feet)
- Botox® injections to block sweat signals
- Microwave therapy or surgical procedures for severe cases

We treat Vitiligo, a condition that causes loss of skin pigment in patches. It’s not dangerous, but it can affect confidence and cause emotional stress. Our dermatology team offers tailored options to slow progression and help restore skin tone.
Vitiligo Symptoms
- White or light patches on skin
- Often symmetrical (both sides of body)
- Hair in affected areas may turn white
- Patches may gradually spread or remain stable
Causes & Risk Factors
- Immune system attacks pigment cells (melanocytes)
- Genetic predisposition / family history
- Triggers: sunburn, stress, skin injury (Koebner effect)
- Associated autoimmune diseases
Diagnosing Vitiligo
- Visual examination by dermatologist
- Wood’s lamp (UV light) to highlight depigmented areas
- Blood tests to check for autoimmune conditions
Treatment Options
- Topical corticosteroids or calcineurin inhibitors
- Phototherapy (narrowband UVB)
- Depigmentation (in extensive cases)
- Skin grafts or melanocyte transplant (in select cases)
- Cosmetic camouflage and makeup
Outlook & Living With It
- No cure, but treatments can slow or reverse patches
- Use sunscreen on depigmented areas (risk of sunburn)
- Emotional support / counseling can help
- Monitor for changes; adjust treatment over time

Prevention is the Best Medicine
Regular skin checks, mole evaluations, and early treatment are essential for long-term skin health. We help you take proactive steps to protect against sun damage, aging, and skin cancer.
Discover the Latest in Skin Health & Beauty
Explore Expert Articles & Skin Care Tips
Stay informed with our latest updates on prevention, treatment, and care — written by our dermatology specialists to help you keep your skin healthy and confident.